How Birth Doulas Are Helping Parents Navigate Coronavirus
Kimberly Sherman felt a pang of uncertainty when she went to the hospital in April to give birth. As a mother of 6-year-old twin boys, this was not her first time. But entering a hospital amid a raging global pandemic left Sherman, a women’s health specialist with the U.S. Department of Health and Human Services, with a feeling of unease.
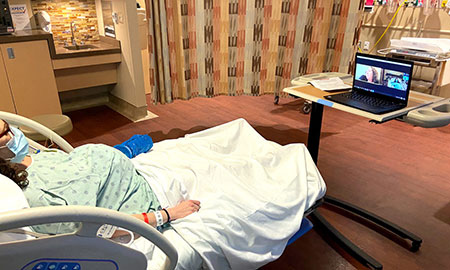
She spent an anxiety-filled two hours, gripped by labor pains, awaiting the results of a COVID-19 test before she could be allowed into the delivery room. The hospital was permitting only one support person to accompany her, and she knew that in choosing her husband, her birth doula could not be with her. So the couple did what a growing number of parents are doing in this crisis: they packed their laptop and took their doula with them virtually.
That voice and face on their laptop screen brought soothing comfort at a time of distress, Sherman recalls, talking them through what to expect, discussing their choices and decisions, and addressing their fears.
“She was a sounding board…that voice, and logical support from start to finish,” Sherman recalls. “[She] never left my virtual side. She heard all the advice the nurses provided and talked me through options for labor support.”
The Shermans’ decision to use a doula to help them navigate the birthing process in a world upended by the coronavirus mirrors that of a growing number of people giving birth during this unusual time. Many, especially those giving birth in hospitals with strict limits on the number of support people allowed in the delivery room, are packing laptops and tablets and inquiring about internet signals to ensure their birth doulas will be at their virtual side. In some cases, birthing persons are even choosing doulas over partners.
“Labor and birth can already be a nerve-wracking experience for many birthing people, and the global pandemic adds to that anxiety,” says Jordan Alam, a Seattle-based independent doula and program coordinator for Open Arms Perinatal Services, which offers community-based support during pregnancy, birth, and early parenting. “Reducing access to support systems and limiting the agency of our clients can heighten the risk for perinatal mental health conditions if we’re not careful.”
Doulas help ease some of the anxiety and stress in patients, especially those giving birth for the first time, by providing education, coping strategies, and emotional and physical support before, during, and after birth. They help parents create a birth plan, which lets the medical team know the patient’s labor and delivery preferences for things such as pain management, postpartum care, and newborn procedures. Doulas advocate on parents’ behalf, often against unnecessary procedures such as cesarean sections, and they coach parents during the birth, suggesting techniques related to positioning and breathing. Heightened concerns over COVID-19 have made all those even more crucial.
Ursula Sukinik, a doula, midwife, and childbirth educator, has overseen almost 20 births virtually since the crisis began. It’s not a new area of practice for her. For six years, the CEO of Birth You Desire, a birth-support organization based in Washington, D.C., has offered virtual services to clients who have moved out of the area.
Like physicians, nurses, and others in the field of medicine, doulas are similarly affected by the paucity of personal protective equipment for in-hospital use—as well as the stress of being in the health care setting. In instances where there are no masks, Sukinik says, doulas are wearing cloth substitutes. They are being fastidious about washing their hands, wiping everything down, to avoid not only contracting the virus themselves, but also to avoid transferring it to parents and newborns.
For doulas connecting virtually, natural challenges come with not being there in person, such as not being able to physically position a laboring parent or having to depend on other cues to offer guidance. Communications can be made more complicated when the muffled voices of professionals are offering instructions through a mask.
Sukinik says it has meant communicating more with partners in the room and having them serve as the missing doula’s eyes, ears, and hands. It means, “saying things like, ‘It looks like this is where the monitor is…can you help me to move her?’” Sukinik says. “Or, ‘that’s not the position I was looking for.’ Partners, she says, are “loving that they get to be the eyes and the ears and the hands when someone else is telling them what to do.”
But while technology has proven vital in filling service gaps in this crisis, people are confronting its limitation not just during labor but afterwards, too. Things such as postpartum visits with doctors via a screen are tricky and can leave new parents feeling uneasy.
“Beyond emotional challenges, there are serious logistical ones,” says Kimberly Sutton, a new mom from Washington, D.C. “I’ve had trouble breastfeeding and have had to turn to telemedicine with breastfeeding consultants to try to help.”
At the guidance of their pediatrician, she says, she rented an infant scale and plans to do all her pediatrician appointments through telemedicine. “My six-week postpartum visit will be done via telemedicine—if at all,” she says.
As everyone—from health care professionals to patients—is doing their part to ensure the safety of all, Sutton says, support looks and feels very different from what new parents might have expected or have been accustomed to. “How am I supposed to know if I’ve recovered from labor and delivery if no doctor looks at me?” she says. “How do I know if her lungs and heart are developing right if no doctor listens to them?”
Doulas describe discharges from hospitals during the crisis as more procedural, cold, and almost impersonal, as some people are being sent home sooner to reduce the risk of their contracting the virus. That and the general concerns over being in a hospital have driven an increase in requests for home births.
Maria Kilkelly, a federal employee, decided to have her first child at home because hospitals in the Washington, D.C. area, where she lives, have been limiting the number of people in labor and delivery to only one person.
She made the switch so she could have a team with her when she delivered her baby. “Along with our doula, we will have a midwife and a birth assistant present as well,” she says.
All these issues can be even more complicated for people of color, who can face medical racism in a country with one of the highest maternal mortality rates in the developed world. What’s more, Black and Brown people have been disproportionately affected by COVID-19 and even before the pandemic, African American people giving birth were experiencing complications and fatalities at higher rates.
For them, Alam says, having access to doulas becomes even more important as changing and shifting hospital policies limit a person’s ability to advocate for the kind of birth they want. The current circumstances, she says, “put them at risk for great re-traumatization when interacting with an overtaxed hospital environment, since we know that even on a good day it can be challenging for people of color to get the appropriate care they need.”

Elon Geffrard, a doula from the Detroit area, holds a baby she helped deliver in March 2017. Photo from Elon Geffrard.
Sherman, who is African American and had a negative birth experience the first time, says she made sure that she and her doula advocated on her behalf with this second birth. “I was also fearful of having (another) bad experience such as not being listened to and even talked down to, which is what happened during our first birth.” Her doula, she says, “wanted to hear about those fears and worked with me to address them.”
Elon Geffrard, a doula of color in the Detroit area, says African American people make up most of her practice, and she has witnessed the obstacles they face in health care—their needs frequently ignored—both before and during this pandemic. While she’s glad to see that reporting on COVID-19 has exposed existing gaps in the health care system, she presses providers to go further to address the systemic issues that result in such disparate care. “There have been discussions about morbidity and mortality during childbirth and the postpartum period, but I’d like to see more effort to mitigate those disparities,” she says. “There’s the acknowledgement, but what do we do to rectify that?”
Geffrard is doing her part by standing up for her clients to identify problems before they surface as a way of correcting these inequities. As a doula, she says, her “role is to lift the voice of my client, to remind them that you have a choice in your care…hospital policy is not law.”
Danielle Hayden is a freelance writer based in Seattle.
This article was republished from YES! Magazine.